Understanding Nephritis vs Nephrotic Syndrome: A Comprehensive Comparison
The realm of nephrology is often filled with intricate terms that require keen distinction for effective diagnosis and treatment. Among the most frequently discussed conditions are Nephritis and Nephrotic Syndrome. Though both affect kidney function, they manifest distinctly in terms of symptoms, underlying causes, and treatments. This article aims to provide a focused exploration of these two conditions, clarifying their differences through expert insights and evidence-based statements.
Key Insights
- Primary Insight with Practical Relevance: Understanding the nuanced differences between Nephritis and Nephrotic Syndrome is critical for accurate diagnosis and tailored treatment plans.
- Technical Consideration with Clear Application: Nephritis primarily involves inflammation of the kidney tissue, while Nephrotic Syndrome involves the excessive loss of protein in the urine.
- Actionable Recommendation: Always consider the full clinical picture, including specific symptoms and lab results, when distinguishing between these conditions.
Definitions and Basic Understanding
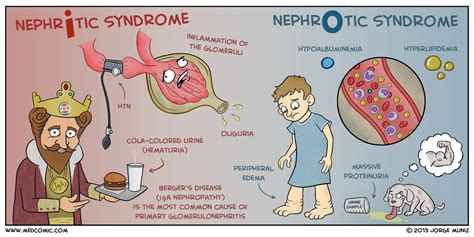
Nephritis and Nephrotic Syndrome are often confused due to their overlapping impacts on kidney health. Nephritis refers to a group of diseases characterized by the inflammation of kidney tissues. This condition can arise from infections, autoimmune disorders, or certain drugs. In contrast, Nephrotic Syndrome is a collection of symptoms including severe swelling, significant protein loss in urine (proteinuria), low blood protein levels (hypoalbuminemia), and high cholesterol levels. While Nephritis specifically indicates kidney inflammation, Nephrotic Syndrome is a syndrome that encompasses a range of symptoms primarily driven by protein loss.
Symptoms and Clinical Presentation
The symptomatic distinction between Nephritis and Nephrotic Syndrome is crucial for healthcare professionals. Nephritis often presents with symptoms such as blood in the urine, swelling in the area around the eyes, joint pain, fever, and fatigue due to the body’s inflammatory response. In contrast, Nephrotic Syndrome typically shows more pronounced signs like generalized swelling (edema), particularly around the ankles and in the abdominal region (ascites), foamy urine due to protein overflow, and significant weight gain due to fluid retention. Though inflammation is a component in Nephritis, Nephrotic Syndrome’s hallmark is the excessive excretion of protein.
It's vital to recognize that while both conditions can lead to significant kidney impairment, the underlying mechanisms and resultant clinical pictures differ markedly. Hence, an accurate diagnosis hinges on meticulous evaluation of these symptom differences.
Can Nephritis lead to Nephrotic Syndrome?
While there isn't a direct causal link, some types of Nephritis, such as Focal Segmental Glomerulosclerosis, can progress to Nephrotic Syndrome if the inflammation leads to significant damage of kidney glomeruli.
How are treatments for Nephritis and Nephrotic Syndrome different?
Treatment approaches vary significantly. Nephritis treatment often focuses on addressing the underlying inflammation, which may involve corticosteroids, immunosuppressants, or antibiotics, depending on the cause. In contrast, Nephrotic Syndrome treatment is more about managing symptoms and includes diuretics, blood pressure medications, and dietary changes to control protein and salt intake.
In summary, Nephritis and Nephrotic Syndrome, while both affecting kidney health, differ substantially in their clinical manifestations, underlying mechanisms, and treatment protocols. A nuanced understanding of these differences is indispensable for healthcare providers to deliver precise and effective care.