Understanding Wet Age-Related Macular Degeneration: Insights, Evidence, and Action
In the vast landscape of ocular health, Wet Age-Related Macular Degeneration (wet AMD) stands out as a formidable adversary. This progressive condition leads to significant vision loss, impacting millions globally. As experts in the field, it’s our duty to demystify its complexities, dissect proven strategies, and arm both patients and professionals with critical insights.
Key insights box:
Key Insights
- Wet AMD primarily occurs due to abnormal blood vessel growth in the retina.
- Anti-VEGF therapy has revolutionized treatment efficacy for wet AMD.
- Early diagnosis and continuous monitoring are critical for managing wet AMD.
Wet AMD: Etiology and Mechanism Wet AMD arises from the leakage and bleeding of abnormal blood vessels (choroidal neovascularization) that sprout under the macula, leading to its deterioration. Risk factors include genetic predisposition, age (usually over 50), and lifestyle choices. The macula, central to our visual field, is rendered dysfunctional when its vasculature is compromised.
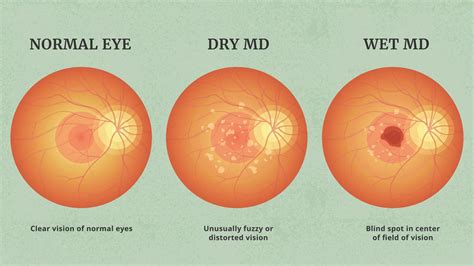
The vascular endothelial growth factor (VEGF) plays a pivotal role in the neovascularization process. Elevated levels of VEGF spur on the formation of fragile blood vessels that disrupt the retinal architecture, contributing to the hallmark symptoms: distorted vision, blurred spots, and central vision loss.
Treatment Landscape: A Paradigm Shift Historically, wet AMD management offered limited hope, primarily focusing on slowing its progression. However, the advent of anti-VEGF therapies has transformed patient outcomes. These agents, targeting the overactive VEGF, inhibit neovascularization and reduce leakage, thus preserving or even improving vision.
For instance, Ranibizumab (Lucentis) and Aflibercept (Eylea) have demonstrated significant efficacy in clinical trials, reducing fluid in the retina and stabilizing visual acuity. Their administration via intravitreal injections necessitates a careful balance, ensuring both efficacy and safety. Despite potential side effects, the benefits often outweigh the risks, marking a significant leap forward in wet AMD treatment protocols.
Management Strategies and Future Directions Managing wet AMD requires a multi-faceted approach encompassing regular ophthalmic evaluations, genetic screening, and lifestyle modifications. Regular follow-ups allow for timely interventions, crucial in mitigating vision loss. Genetic counseling may also aid in understanding hereditary risk factors, allowing for preventive measures.
Innovations in treatment are underway, with new anti-VEGF agents on the horizon. Photodynamic therapy (PDT) and sustained-release implants provide alternative modalities, ensuring a robust pipeline of treatment options.
FAQ section:
What are the primary symptoms of Wet AMD?
The primary symptoms of wet AMD include distorted vision, blurred spots, and a progressive loss of central vision. These changes often manifest subtly at first but become more pronounced over time.
Is Wet AMD reversible?
Unfortunately, wet AMD does not have a cure. However, with early intervention and ongoing treatment, significant vision loss can be mitigated, and some patients experience stabilization or even slight improvements in vision.
In closing, wet AMD presents significant challenges, but armed with a nuanced understanding, evidence-based treatments, and proactive management, both patients and healthcare providers can navigate this complex condition more effectively. The journey towards optimal visual health, while ongoing, is one marked by hope, innovation, and informed action.